POTS flare-up: Triggers, symptoms, and how to cope
September 2, 2025

- A POTS flare-up is when symptoms temporarily worsen, often triggered by stress, illness, heat, dehydration, or hormonal changes.
- Flare-ups can last anywhere from a few hours to several weeks, depending on the individual.
- Using tools like the Human Health app makes it easier to spot patterns, share information with your doctor, and build better coping strategies.
Living with postural orthostatic tachycardia syndrome (POTS) often means symptoms can change from one day to the next. Some days feel manageable, while others feel particularly challenging, with everyday tasks becoming harder to cope with.
These flare-ups don’t usually happen at random. Many people find they are linked to triggers like illness, dehydration, heat, stress, or hormonal changes. Over time, noticing and tracking these patterns can make it easier to understand what sets symptoms off and how to manage them.
In this article, we’ll look at what happens during a POTS flare-up, how long they can last, common triggers, and practical ways to track and cope with them.
What happens during a POTS flare-up?
Common POTS symptoms include lightheadedness when standing, fatigue, brain fog, and sometimes dizziness or near-fainting.
One of the hallmark signs is a significant increase in heart rate when moving from lying down to standing, often rising by 30 beats per minute or more within about 10 minutes of standing up.
You may be experiencing a POTS flare-up if your symptoms suddenly worsen beyond your usual baseline. You might find they become more intense and disruptive.
How long do POTS flare-ups typically last?
Flare-ups vary widely. For some people, they may be brief and mild. For others, they may be more severe and long-lasting.
Some people notice their symptoms ease within a few hours, while others experience setbacks that last for days or even weeks. Factors like illness, hormonal changes, and stress levels can all influence recovery time.
Common triggers that can lead to a flare-up
POTS affects people differently, so triggers can vary widely from person to person. What causes a flare for someone else may not affect you in the same way. Because of this, tracking symptoms and daily habits can be helpful in identifying personal patterns.
That said, certain triggers are reported more often by people living with POTS. Flare-ups commonly occur when the body is under additional strain, such as during illness, dehydration, heat exposure, hormonal changes, or periods of physical or emotional stress.
Illness or infection
Even a minor infection (like a cold or stomach bug) can cause POTS symptoms to worsen. Recovery may also take longer than in people without the condition.
Heat exposure
Warm environments can make it harder for the body to circulate blood effectively, which may cause less blood to reach the heart and brain.
Hot weather, saunas, or even long, hot showers may increase dizziness and tiredness for some people with POTS.
Research shows that heat can lower the body’s ability to stay upright by affecting how blood vessels tighten and relax.
Dehydration
When you don’t get enough fluids or electrolytes, blood volume can drop. This can make symptoms like lightheadedness and a fast heartbeat worse in POTS.
Dehydration may come from sweating, not drinking enough water, or illnesses that cause fluid loss. Staying mindful of hydration levels can reduce the likelihood of a POTS flare-up.
Hormonal changes
Many women report flares tied to the menstrual cycle, pregnancy, or menopause, when changes in estrogen and progesterone affect blood volume and vessel tone. These shifts can make otherwise manageable symptoms much harder to handle during certain times of the month.
Stress and exertion
Periods of high emotional or physical stress (including intense exercise or anxiety) are often cited as triggers for worsening fatigue, dizziness, or palpitations in POTS.
Symptoms tracking for staying on top of flare-ups
Symptoms and flare-ups can often feel unpredictable in POTS. That’s why tracking symptoms is helpful. It turns scattered experiences into clear patterns you can act on.
Over time, these insights help you better understand your body and anticipate flare-ups. Recognizing potential patterns and triggers can lead to more productive conversations with your healthcare provider.
Method #1: Human Health app
The Human Health app was built for complex conditions like POTS.
You can log daily symptoms, flare severity, and possible triggers all in one place. Over weeks and months, the app organizes your entries into clear trends, helping you see what makes symptoms better or worse. With one tap, you can export a practitioner-ready PDF summary, transforming vague memories into data-backed insights that support better care decisions.
Method #2: Symptom journal
Recording observations about your flare-ups in a notebook or digital diary can be a helpful starting point. For example, you might note when symptoms worsen and what was happening around that time. Recording factors such as sleep, meals, hydration, activity levels, stress, or environmental conditions can help reveal useful patterns.
The drawback is that journals are harder to analyze over time. They are also difficult to share in a structured way with your doctor.
Method #3: Wearables and devices
Smartwatches and fitness trackers can add objective data to your records. By capturing heart rate changes, activity levels, or sleep patterns, they provide useful context alongside your symptom notes. When reviewed together, this data can help you and your healthcare provider better understand when symptoms worsen and what might be contributing to flare-ups.
While any form of tracking is better than none, using a platform designed for complex conditions makes the process easier and more impactful. The Human Health app combines the flexibility of a journal with structured reports and insights you can actually act on, helping you feel more in control of your flare-ups.
{{inline-cta-1}}
What to do during a POTS flare-up
During a flare-up, even simple activities can feel overwhelming. Over time, tracking symptoms and triggers can help you better understand what’s happening in your body and what tends to help during these periods.
In the moment, small supportive adjustments can make a flare more manageable. While everyone’s approach is different, many people with POTS find the following strategies helpful:
Rest and pacing
POTS symptoms often worsen when you stay upright for long periods because the body has difficulty regulating blood flow and heart rate when standing. During a flare, slowing down and pacing activities can help prevent symptoms from escalating.
Some people also find temporary relief by resting in a reclined position or taking breaks between tasks to allow their body time to recover.
Cooling and hydration
Staying cool and hydrated can also help you manage flare-ups.
Using a fan or a cooling towel may reduce your dizziness or tiredness. Sipping a cool drink may also help. Drinks that include electrolytes can help replace fluids, especially if dehydration plays a role.
Supportive positioning
Changing your position can sometimes ease symptoms during a flare-up. Sitting or reclining, or elevating your legs, may help blood flow return toward the heart and reduce dizziness or a racing heart.
Compression garments can also support circulation. Research suggests that full compression may minimize the increase in heart rate that occurs when standing in people with POTS.
Quick POTS flare-up toolkit
- Refillable water bottle or electrolyte drink
- Cooling towel, handheld fan, or ice pack
- Compression socks or leggings
- Reclining chair or pillow for leg elevation
- Notebook or app to log flare details
Lifestyle strategies for POTS flare-ups
Managing POTS over the long term means building habits that support stability and resilience between flares. These approaches don’t prevent flares entirely but may help reduce their impact.
Steady routines
Regular sleep, meals, and daily rhythms can help create a steadier baseline for your body. They can also boost your general well-being and reduce the risk of stress.
Staying in tune with your body and monitoring how symptoms change over days, weeks, and months can make it easier to notice patterns and respond early when symptoms begin to worsen.
Hydration and salt tracking
Staying well hydrated and maintaining adequate salt intake are commonly recommended strategies for supporting blood volume in people with POTS.
Some people choose to track their fluid and salt intake alongside symptoms to see how these factors influence how they feel.
Gentle, consistent activity
While exercise can feel difficult with POTS, regular movement can support circulation and overall conditioning. Many people benefit from starting with low-intensity or seated activities and gradually building tolerance over time, ideally with guidance from a clinician familiar with POTS.
When to seek medical attention during a flare-up
It’s important not to dismiss severe or unusual symptoms as “just another flare-up.”
If you experience fainting, chest pain, extreme shortness of breath, or symptoms that feel very different from your usual pattern, seek medical care right away. Only a doctor can rule out other causes and ensure your safety.
What to tell your doctor during a flare-up
- When the flare started and how long it has lasted
- The main symptoms and how they differ from your baseline
- Any potential triggers you noticed (illness, stress, heat, dehydration)
- Notes or symptom logs from your tracking app or journal
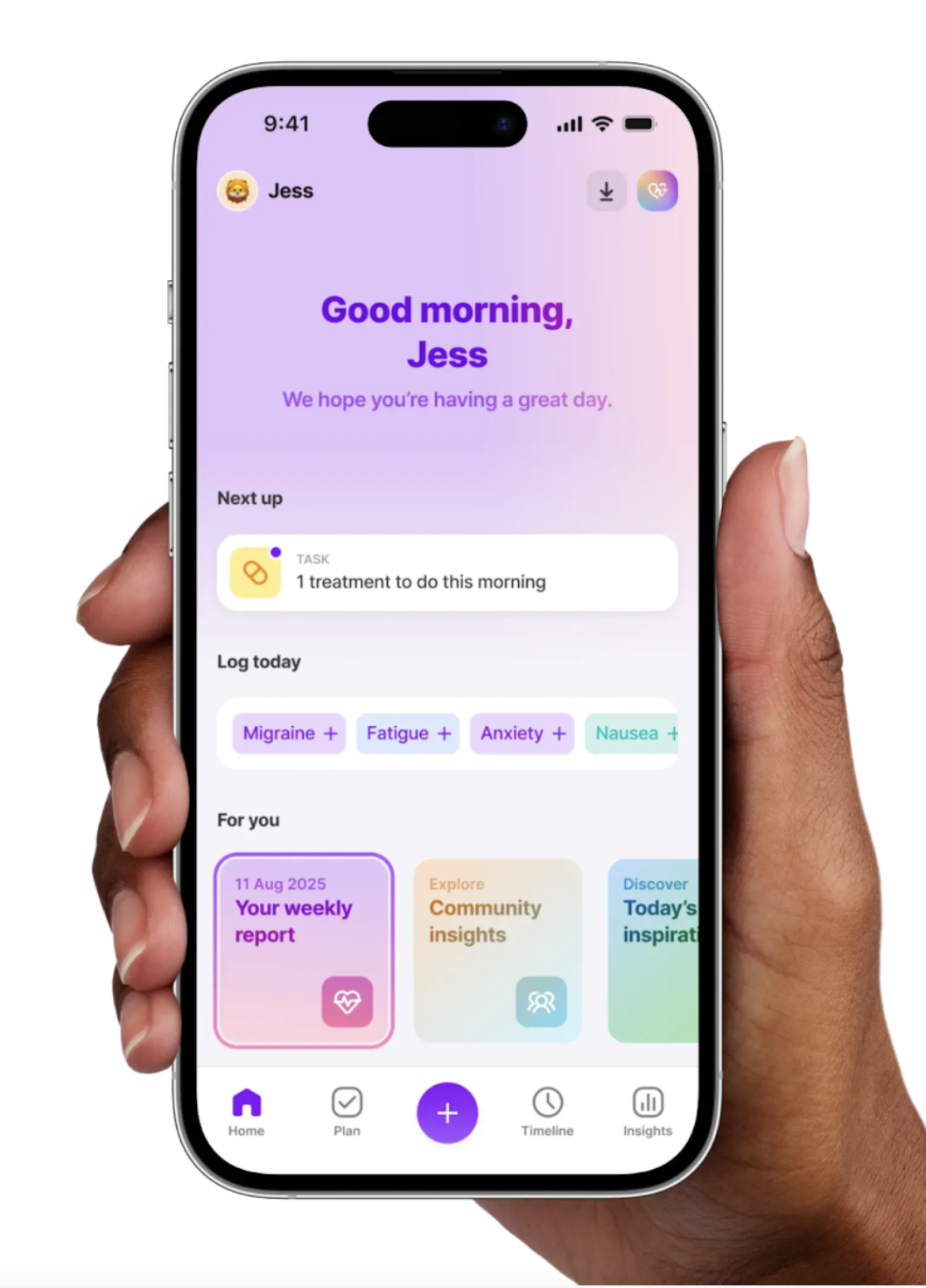
How the Human Health app can help you manage POTS flare-ups
Flare-ups often feel unpredictable and frustrating. The Human Health app helps take away some of that uncertainty by showing you what is really happening over time. Logging symptoms, treatments, and routines builds a clear record that you can look back on, rather than guessing.
With practitioner-ready summaries, you arrive at appointments prepared. This makes it easier for your doctor to see the full picture. Tracking habits like hydration, salt intake, exercise, and compression wear also gives you clarity on what supports you best, so you can focus energy where it matters most.
The Human Health app gives you a long-term support system. It helps you move from feeling reactive to feeling more in control.
Frequently Asked Questions:
1. Can emotional stress alone cause a POTS flare-up?
Yes. Many people report that emotional stress can trigger or worsen symptoms, though the intensity and duration vary from person to person.
2. Should I adjust my exercise routine during a flare-up?
It’s often helpful to reduce intensity or take a break during a flare-up, but only a healthcare provider can guide what’s safe for you.
3. Is it normal for flare-up triggers to change over time?
Yes, triggers may shift depending on factors like hormones, illness, or lifestyle. Tracking the circumstances surrounding your flare-ups (like hydration, health, well-being, diet, exercise, stress levels, and menstrual cycle) helps you notice and adapt to these changes.
Sources:
- National Library of Medicine: Cognitive and Psychological Issues in Postural Tachycardia Syndrome
- National Library of Medicine: Menstrual Cycle Affects Renal-Adrenal and Hemodynamic Responses during Prolonged Standing in the Postural Orthostatic Tachycardia Syndrome
- National Library of Medicine: Experiences of living with postural tachycardia syndrome
- National Library of Medicine: Postural orthostatic tachycardia syndrome (POTS) and other autonomic disorders after COVID-19 infection: a case series of 20 patients
- Heart and Mind: Psychological stress in postural orthostatic tachycardia syndrome: A pilot pre-COVID survey
- National Library of Medicine: Mechanisms of orthostatic intolerance during heat stress
- National Library of Medicine: Diagnosis and management of postural orthostatic tachycardia syndrome
- ScienceDirect: Oral and intravenous hydration in the treatment of orthostatic hypotension and postural tachycardia syndrome
- JACC Journals: Compression Garment Reduces Orthostatic Tachycardia and Symptoms in Patients With Postural Orthostatic Tachycardia Syndrome
- National Library of Medicine: Exercise and Non-Pharmacological Treatment of POTS
- Australian POTS Foundation: Living with POTS
Disclaimer: Human Health is a health tracking platform and does not provide medical advice, diagnosis, or treatment. The information below is for educational purposes only and is not a substitute for professional medical care. Always consult your doctor or healthcare provider with questions about your health.
This is a div block with a Webflow interaction that will be triggered when the heading is in the view.

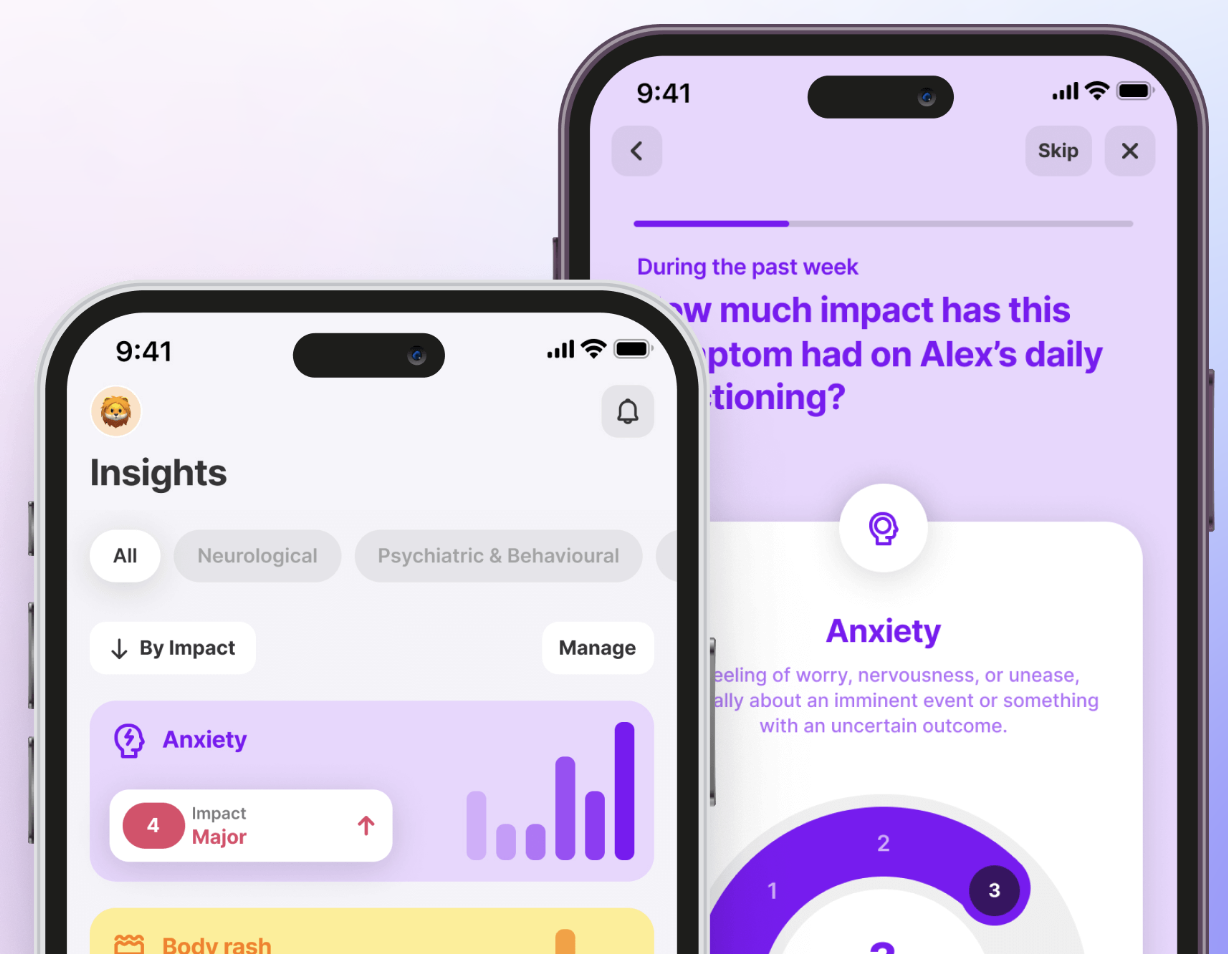
Doctors Dismissing You? The Human Health App Doesn't!
Inside the app, you can track all your symptoms, medications, flare ups & more. The app also provides you with insights, so you gain the clarity you need.








.jpg)




.png)

