Dysautonomia vs POTS: Shared symptoms & differences
October 1, 2025

- Dysautonomia is a broad term describing dysfunction of the autonomic nervous system, while POTS (postural orthostatic tachycardia syndrome) is one specific type of dysautonomia.
- Both conditions may share symptoms like dizziness, fatigue, and heart rate changes, but they are not the same condition.
- POTS is primarily identified by a rapid heart rate increase when going from lying down to standing.
- Using the Human Health App to track daily symptoms, treatment responses, and triggers can help you and your healthcare provider spot meaningful patterns and guide care discussions.
When it comes to dysautonomia vs POTS, many people wonder whether they are dealing with the same condition or two separate health issues.
In this article, we’ll walk through their shared symptoms, the differences that matter most, how doctors diagnose them, and what current treatments look like. You’ll also learn how tracking with the Human Health app can help you and your provider connect the dots and make more informed care decisions.
What is the link between POTS and dysautonomia?
Dysautonomia refers to any disorder involving altered autonomic nervous system (ANS) function. The ANS controls functions you don’t usually think about, like heart rate, blood pressure, digestion, and temperature regulation.
Postural orthostatic tachycardia syndrome (POTS) is a specific form of dysautonomia. It is characterized by an excessive increase in heart rate (tachycardia) when moving from lying down to standing up.
In other words, all POTS cases fall under dysautonomia, but not all dysautonomia is POTS.
This connection matters because understanding whether symptoms are caused by POTS or another form of dysautonomia can guide the right diagnosis and management approach.
Symptom overlap in POTS and dysautonomia
Some of the same symptoms occur in POTS and other types of dysautonomia. This can sometimes make diagnosis challenging.
Tracking symptoms consistently gives you and your healthcare provider a clearer view of how your condition is affecting you. Recognizing patterns over time is often the first step toward an accurate diagnosis and better management.
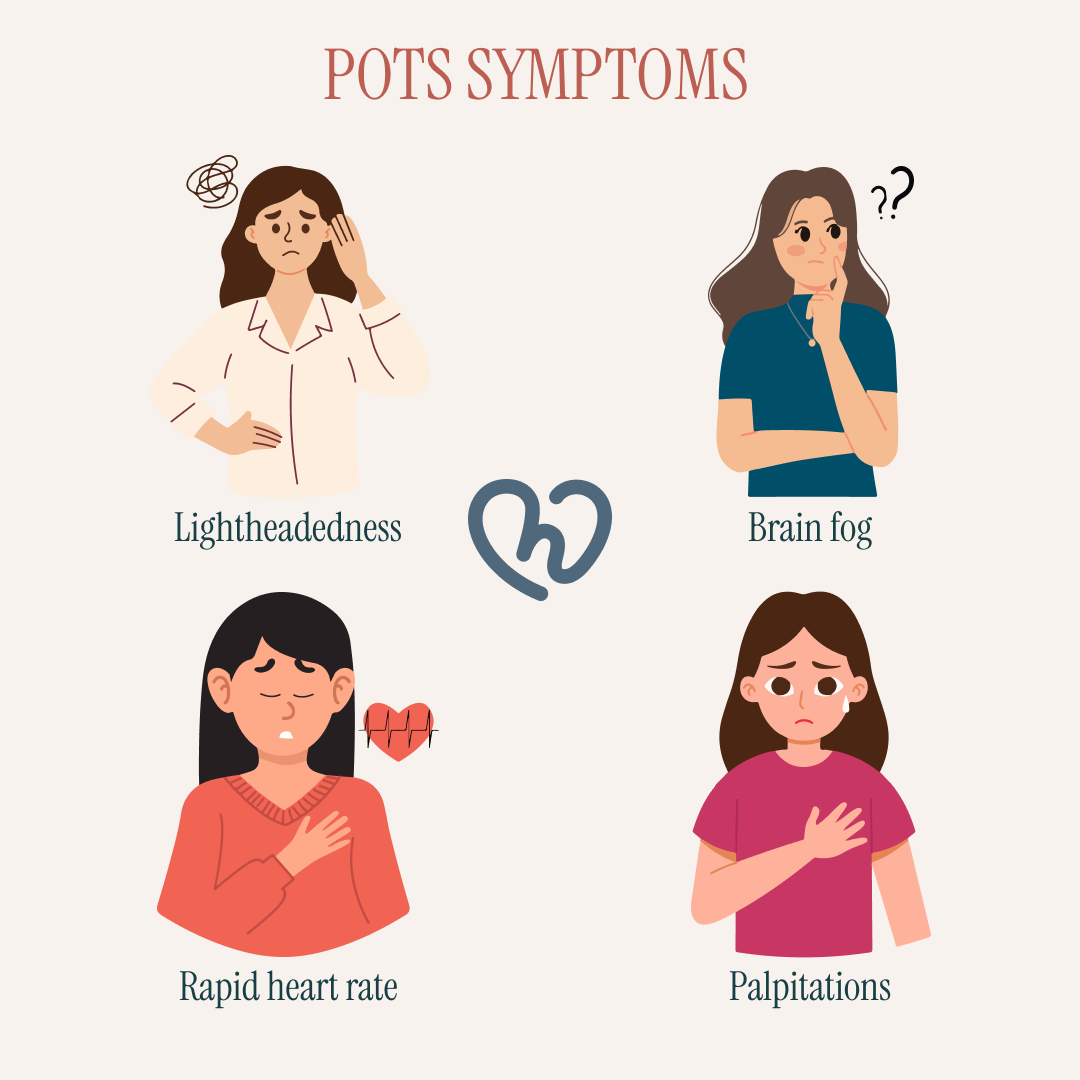
Some symptoms that may overlap include:
Dizziness and lightheadedness
Problems with blood pressure and circulation can make people feel dizzy or lightheaded, particularly when standing up. In some cases, this leads to fainting or feeling close to fainting.
Fatigue
Fatigue is common in POTS and many other forms of dysautonomia. People often describe a deep, persistent tiredness that isn’t fully relieved by rest and can make everyday activities harder to manage.
Brain fog
Many people with POTS and other forms of dysautonomia describe episodes of “brain fog.” This can feel like trouble concentrating, slower thinking, or difficulty finding the right words.
Research suggests these cognitive symptoms may become more noticeable when standing or upright, when changes in circulation and autonomic activity can affect how the brain functions.
Rapid heart rate
A rapid heartbeat when standing is the hallmark of POTS, though other forms of dysautonomia can also cause elevated heart rate in certain situations.
Potential causes of POTS and dysautonomia
Researchers are still working to fully understand what causes these conditions. In many cases, several factors may be involved rather than a single clear cause.
This highlights how complex these conditions can be. Because triggers and underlying factors vary widely, tracking symptoms and health history can help your healthcare provider piece together the bigger picture and guide more personalized care.

POTS
POTS can develop suddenly or gradually.
In some people, symptoms begin after a major stress on the body, such as a viral illness, surgery, pregnancy, or physical trauma. In others, symptoms appear more gradually over time.
Some people with POTS also have related conditions such as joint hypermobility or connective tissue disorders, including hypermobile Ehlers–Danlos syndrome. Family history may also play a role in some cases.
If you’ve noticed joint hypermobility or flexible joints alongside POTS-like symptoms, the hypermobile Ehlers-Danlos (hEDS) quiz can help you reflect on your experiences and explore whether hypermobility might be connected to autonomic symptoms.
Other dysautonomia conditions
Dysautonomia can develop for many different reasons. In some people, it appears on its own. In others, it occurs as a secondary condition linked to another illness, such as diabetes, autoimmune disease, or neurological disorders.
Understanding possible causes can help guide medical evaluation and management, but identifying the exact cause is not always straightforward.
POTS vs dysautonomia: What’s the difference?
Not all types of dysautonomia present the same way.
The differences usually come down to how symptoms appear and what happens in the body when someone changes posture or experiences certain triggers.
Changes when standing
One defining feature of POTS is a significant increase in heart rate when moving from lying down to standing. In adults, this is typically a rise of 30 beats per minute or more within 10 minutes of standing, without a significant drop in blood pressure.
Because of this circulation pattern, many people with POTS notice symptoms such as dizziness, palpitations, or fatigue when they are upright.
Other dysautonomia conditions may affect circulation differently. Some disorders cause blood pressure to drop when standing, a condition known as orthostatic hypotension, which can lead to dizziness or fainting.
Different underlying conditions
Some types of dysautonomia mainly affect circulation, while others involve multiple body systems.
For example, neurally mediated syncope can cause fainting when changes in heart rate and blood pressure briefly reduce blood flow to the brain. Other conditions, such as orthostatic hypotension, mainly involve drops in blood pressure when standing.
Because these conditions affect the same regulatory system, their symptoms can sometimes look similar, even though the underlying causes may be different. Understanding how blood pressure behaves in conditions like POTS can help clarify these differences. You can learn more in our guide to POTS and blood pressure.
{{inline-cta-1}}
Age and onset patterns
POTS most often appears in teens and younger adults, and it is particularly common in women. Symptoms frequently begin in adolescence or early adulthood, although the condition can develop at other ages as well.
Other forms of dysautonomia can develop later in life, especially when autonomic nerve dysfunction occurs as part of another medical condition. In adults, dysautonomia may be secondary to illnesses such as diabetes, autoimmune disorders, or neurological diseases. It may also result from nerve injury or certain medications.
Some dysautonomia conditions are also linked to neurodegenerative diseases such as Parkinson’s disease. With these conditions, damage to the nervous system can interfere with the body’s ability to regulate functions like blood pressure, digestion, and temperature.
Because dysautonomia can arise from different causes and at different stages of life, careful evaluation is important. Symptoms may look similar across conditions, but understanding the underlying cause helps clinicians determine whether someone is experiencing POTS or another type of autonomic disorder.
How doctors diagnose POTS and other dysautonomia conditions
Diagnosing autonomic disorders can be challenging because symptoms such as dizziness, fatigue, and rapid heart rate can occur in many different conditions. People with POTS and related conditions often face delays or misdiagnoses.
POTS
POTS is usually identified by a specific change in heart rate when someone moves from lying down to standing.
Doctors typically look for:
- A sustained increase in heart rate of at least 30 beats per minute within 10 minutes of standing
- Symptoms that worsen when upright, such as dizziness, lightheadedness, fatigue, or palpitations
- No significant drop in blood pressure
This response is often measured using a tilt-table test or by monitoring heart rate and blood pressure while a person moves from lying down to standing.
Other dysautonomia conditions
The diagnostic process for other types of dysautonomia can vary depending on the suspected condition.
Doctors may use tests that evaluate how the autonomic nervous system regulates functions such as:
- Heart rate
- Blood pressure
- Sweating
- Circulation
Diagnosis also usually involves reviewing medical history, symptoms, and possible underlying conditions, such as diabetes, autoimmune disease, or neurological disorders.
Why tracking symptom patterns matters
Diagnosing autonomic conditions often depends on identifying patterns, such as when symptoms occur and how heart rate changes when standing.
Research suggests that wearable devices and digital tools can help capture heart-rate patterns and other physiological signals during daily life, providing useful context alongside clinical testing.
Tracking symptoms like dizziness, fatigue, and rapid heart rate can help you and your healthcare provider see those patterns more clearly. The Human Health app lets you record these changes and share summaries during medical appointments.
Management advice for POTS and dysautonomia
Researchers are still trying to understand POTS and other dysautonomia conditions.
While there’s no single cure, many people find ways to reduce the impact of symptoms with consistent management strategies.
#1: Track symptoms and patterns
Keeping a detailed symptom log is one of the most practical steps you can take.
With the Human Health App, you can track dizziness, fatigue, and heart rate changes, then export PDF summaries for your healthcare provider. Over time, this makes it easier to spot patterns and triggers that might otherwise be missed.
#2: Focus on hydration and salt intake
Increasing fluid and salt intake, in particular, adopting a high‐sodium diet, has been shown to increase plasma volume and reduce upright tachycardia in POTS patients.
Only make these changes with guidance from your doctor.
#3: Gradual exercise and movement
For some people with POTS, gentle exercise introduced gradually can help improve symptoms.
Doctors often recommend starting with activities that can be done sitting or lying down, such as swimming, rowing, or using a recumbent bike. As fitness improves, exercise can slowly become more upright.
Structured exercise programs have been shown to improve circulation and quality of life in people with POTS.
#4: Lifestyle adjustments
Compression garments have been shown to reduce orthostatic tachycardia and improve symptoms in people with POTS. Pacing daily tasks also helps conserve energy.
Recording these strategies in the Human Health app, alongside how they affect your symptoms, gives you and your provider clearer insight into what’s working.
Management involves trial and error. By combining medical advice with consistent tracking, you can identify strategies that ease your symptoms and bring more stability to daily life.
Manage POTS and dysautonomia with the Human Health app
POTS is one type of dysautonomia, but many autonomic conditions share similar symptoms. Because dizziness, fatigue, and heart rate changes can overlap across conditions, identifying patterns over time is often an important part of reaching an accurate diagnosis and finding the best management approach for you.
Tracking your own experiences can help make those patterns clearer.
With the Human Health app, you can log symptoms, track them alongside treatments or lifestyle notes, and export clear reports to share with your healthcare provider.
Over time, consistent tracking can turn scattered symptoms into useful insights, helping you and your care team better understand what’s happening and decide on the next steps.
Start tracking today with the Human Health app.
Disclaimer: Human Health is a health tracking platform and does not provide medical advice, diagnosis, or treatment. The information in this article is for educational purposes only and is not a substitute for professional medical advice. Please consult a qualified healthcare provider about your specific situation.
References
- The Diagnostic Journey of Dysautonomia Patients: Insights from a Patient-Reported Outcome Study (2025)
- Postural Orthostatic Tachycardia Syndrome (2023)
- Brain fog in neuropathic postural tachycardia syndrome may be associated with autonomic hyperarousal and improves after water drinking (2022)
- Narrative Review of Postural Orthostatic Tachycardia Syndrome: Associated Conditions and Management Strategies (2023)
- Clinical Evidence of Dysautonomia, The National Library of Medicine
- Postural Tachycardia Syndrome (POTS), National Institute of Neurological Disorders and Stroke
- Dysautonomia, The Dysautonomia Project
- Orthostatic Hypotension (2025)
- Autonomic Dysfunction (2023)
- Dysautonomia: a common comorbidity of systemic disease (2025)
- Wearable Devices for Remote Monitoring of Heart Rate and Heart Rate Variability—What We Know and What Is Coming (2022)
- Effect of High Dietary Sodium Intake in Patients With Postural Tachycardia Syndrome (2021)
- Exercise and Non-Pharmacological Treatment of POTS (2018)
- Compression Garment Reduces Orthostatic Tachycardia and Symptoms in Patients With Postural Orthostatic Tachycardia Syndrome (2021)
This is a div block with a Webflow interaction that will be triggered when the heading is in the view.

Track Your Symptoms In Our App
With the Human Health App - you can better understand yourself and your needs, allowing you to talk to your providers with confidence & be heard.








.jpg)





.png)

